Effects of Diabetes Home-Visiting Healthcare Simulation Education on Nursing Students Using Virtual Reality
Copyright ⓒ 2025 The Digital Contents Society
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-CommercialLicense(http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.

Abstract
This study aimed to examine the effects of virtual reality (VR)-based diabetes home-visit healthcare simulation on nursing students’ learning immersion, clinical judgment ability, and clinical competency with a nonequivalent control group in pre-posttest quasi-experimental design. The experimental group was subjected to VR-based simulation, whereas the control group received standardized patient-based simulation. The participants were nursing students from a university located in City D, with 34 students in the experimental group and 29 in the control group. The results showed that both groups demonstrated significant post-intervention improvements in learning immersion, clinical judgement ability, and clinical performance. Additionally, a statistically significant difference was found between the groups in clinical judgement ability scores. These findings provide foundational evidence for selecting simulation education strategies aligned with clinical training goals and contribute to diversifying instructional approaches for a meaningful nursing education.
초록
본 연구는 가상현실 기반 당뇨병 방문건강관리 시뮬레이션 교육이 간호대학생의 학습몰입, 임상판단 능력, 임상수행능력에 미치는 효과를 검증하기 위해 대조군 비동등성 전후 유사실험 연구를 시행하였다. 본 연구에서 실험군은 가상현실 기반 당뇨병 방문건강관리 시뮬레이션을, 대조군은 표준화 환자 기반 시뮬레이션을 제공받았다. 연구대상은 D시에 소재한 일개 대학 간호학과 재학생으로 최종 실험군 34명, 대조군 29명이 참여하였다. 본 연구결과 두 군 모두 시뮬레이션 학습 몰입, 임상판단 능력, 임상수행능력이 사후 유의하게 향상하였으며, 두 군의 차이 검증에서는 임상판단 능력이 통계적으로 유의한 차이가 있는 것으로 나타났다(t=2.49, p=.015). 따라서 본 연구는 임상실습 교육의 목표와 학습 환경 특성을 고려하여 적절한 시뮬레이션 교육법을 선택하는데 기초자료를 마련하였으며 임상실습 교육 방법의 다양성을 확보하는데 기여하였다는 점에서 의의가 있다.
Keywords:
Virtual-Reality, Diabetes, Home-Visiting Healthcare, Simulation, Standardized Patient키워드:
가상현실, 당뇨병, 방문건강관리, 시뮬레이션, 표준화환자Ⅰ. Introduction
1-1 Background
Diabetes is one of the most prevalent chronic diseases, and its incidence continues to rise globally. In Korea, the prevalence of diabetes reached 12.5% in 2022, marking a 4.8% increase since 2001[1]. Diabetes is a condition in which blood sugar levels are not properly controlled[2]. It can cause serious complications such as heart, blood vessel, and kidney problems[2]. As a result, the economic and social burden of diabetes continues to increase[2]. Diabetes management is difficult to cure and requires lifelong continuous treatment and self-management[2]. Therefore, it is important to help patients understand their disease and practice active self-management along with drug treatment[3]. Various diabetes management projects and education programs are being operated at the national and community levels[4]. Home-visiting healthcare provided at public health centers is an effective approach to improving the self-management ability of patients with chronic diseases and inducing continuous health management[4].
With the increasing diversity of community health needs, there is a greater demand for community nursing practice education. Such education must cover the knowledge, attitudes, and skills required for home-visiting healthcare for patients with chronic diseases, including diabetes[5]. Nursing students recognized the high need for home-visiting healthcare for diabetes and simulation-based education, and there was a high demand for systematic education programs[5].
Recently, the healthcare environment has been rapidly changing. As awareness of patient safety and rights has increased, opportunities for nursing students to perform nursing skills directly in clinical settings have decreased. As a result, clinical practice has shifted to an observation-based format[6],[7]. Community visiting health management practice education must include environmental and lifestyle assessments and customized health education for the target population. To implement this, simulations are being applied in a mixed manner using various types, such as standardized patient(SP)-based mid-fidelity simulations, role-playing, and low-fidelity simulations including simple mannequins[8].
Research has shown that SP simulation is more effective than low-fidelity methods in terms of knowledge, communication skills, and satisfaction with simulation design[9]. However, SP-based simulation education has several limitations. In order for learners to fully experience the emotions and sense of immersion that occur during patient interactions in clinical settings, it is necessary to provide the simulated patients with detailed pre-training on patient characteristics, disease conditions, and behavioral patterns[10]. Additionally, recreating a realistic clinical environment requires substantial investment in terms of cost, personnel, and time. Consequently, SP simulation education has inherent limitations in implementing the non-specific and diverse clinical responses of the subjects[10].
To complement these limitations, head-mounted display (HMD)-based virtual-reality (VR) simulation content is being developed[11]. VR-based education can reproduce realistic clinical situations and provide learners with repeated learning opportunities[12]. It also offers a safe learning environment and promotes self-directed learning by allowing manipulation of subjects' physical reactions, conversation content, and unexpected situations in the simulation[12].
Currently, various educational contents utilizing VR are continuously being developed. Previous studies have shown that VR-based education increases learners’ immersion in simulation and improves communication skills, critical thinking, clinical judgment, and clinical performance[13]. Learning immersion in simulation refers to a state in which learners are immersed in learning and are interested in learning itself[14], and it has been shown to promote direct thinking and experience beyond simple observation[15]. In particular, learning immersion in simulation practice can be considered an important variable that can increase learners' understanding of the role of nurses and develop nursing practice competencies required in clinical settings[15]. In medical settings, nurses are required not only of simple skills but also of clinical judgment ability necessary for decision-making in complex and urgent clinical settings[16]. This clinical judgment ability is a core competency of nurses that can be improved through the stages of cognition-understanding-response–reflection when solving problems[16]. Clinical competency is the ability to competently perform nursing roles in complex clinical situations based on learned knowledge, attitudes, skills, and judgments[17]. Therefore, in nursing education, there is a continuing need for research on VR-based simulation education to enhance nursing students’ learning immersion, clinical judgment, and clinical competency.
Most HMD-based VR simulation contents are focused on hospital-centered or basic nursing fields such as anatomy education[18], neonatal nursing[19]. In cantrast, HMD-based VR simulation programs for community-centered chronic disease management have rarely been developed. Accordingly, research is needed to develop and evaluate the effects of VR-based diabetes home-visiting healthcare simulation education. Therefore, this study aims to compare VR-based simulation education with SP simulation education to examine their effects on nursing students’ learning immersion, dlinical judgment ability, and clinical competency in diabetes home-visiting healthcare, and to provide evidence for a more effective nursing educational program.
1-2 Purpose
The purpose of this study was to compare and analyze the effects of VR-based diabetes home-visiting healthcare simulation and SP-based home-visiting healthcare simulation education on learning immersion, clinical judgment ability, and Clinical competency of nursing students.
1-3 Hypotheses
- Hypothesis 1. The experimental group receiving the VR simulation-based chronic disease home-visiting healthcare simulation education program is expected to exhibit significantly different learning immersion scores compared to the control group receiving SP-based simulation.
- Hypothesis 2. The experimental group is expected to exhibit significantly different clinical judgment ability scores compared to the control group.
- Hypothesis 3. The experimental group is expected to exhibit significantly different clinical competency scores compared to the control group.
Ⅱ. Methods
2-1 Research Design
This study is a quasi-experimental study that applied a nonequivalent control group pre- and post-test design to confirm the effectiveness of a VR simulation-based diabetes home-visiting healthcare simulation education program for nursing students.
2-2 Participants and Data Collection
The subjects of this study were fourth-year students enrolled in the Department of Nursing at a university. They had previously taken a community nursing theory course and had no prior experience with a simulation training for chronic disease home healthcare. The exclusion criteria for the subjects were students who had experience participating in a VR-based simulation training for chronic disease home healthcare, students on leave of absence, and students who experienced side effects such as motion sickness when using VR.
The number of subjects was analyzed using G*Power 3.1.9. The number of subjects analyzed using two independent t-tests was calculated to be a minimum sample size of 42 when applying a significance level of .05, a power of 0.80, and an effect size of 0.89. The effect size applied the clinical competency of a previous study[11], and considering the dropout rate, a total of 70 subjects were selected, with 35 in the experimental group and 35 in the control group.
The data collection period was from October 11 to October 25, 2023. During the period, the researcher confirmed whether the nursing students met the selection criteria, and the intervention was conducted in different simulation locations for the experimental and control groups to prevent the diffusion of the intervention effect. The experimental and control groups recruited 35 people each, but due to personal circumstances and poor responses, data from 34 people in the experimental group and 29 people in the control group were ultimately used for the analysis.
2-3 Research Instruments
Learning immersion was measured using a learning immersion tool developed by Ko[14], which was modified and supplemented by this researcher adapted for this study. This tool consists of 16 items, and is composed of a 5-point Likert scale with 1 point for ‘not at all’, 2 points for ‘no’, 3 points for ‘average’, 4 points for ‘yes’, and 5 points for ‘very much so’. Scores range from 16 to 90, with higher scores indicating greater learning immersion. At the time of development, the Cronbach’s α of the tool was .89[14], and the Cronbach’s ⍺ value of this study was .97.
Clinical judgment ability was measured using the clinical judgment rubric tool developed by Lasater[20], and the Korean version of the Lasater Clinical Judgment Rubric tool developed by Shim & Shin[21] was used. This tool consists of 11 items in 4 areas and 11 subareas. Each item is composed of a 4-point Likert scale with 1 point for ‘very poor’, 2 points for ‘poor’, 3 points for ‘good’, and 4 points for ‘very good’. The score range is 11 to 44 points, and a higher score indicates a higher clinical judgment. Cronbach’s α at the time of development of the Korean version of the tool was .88[21], and the Cronbach’s ⍺ value of this study was .94.
Clinical competency was measured using a tool developed by Lee et al.[22], which was modified and supplemented by Kim et al.[23]. This tool consists of a total of 34 items. Each item is rated on a 5-point Likert scale: 1 point for ‘very poor’, 2 points for ‘slightly poor’, 3 points for ‘average’, 4 points for ‘slightly good’, and 5 points for ‘very good’. The score range is 34 to 170 points, with a higher score indicating a higher level of Clinical competency. The Cronbach’s ⍺ value at the time of tool development was .96[22], and the Cronbach’s ⍺ value in this study was .98.
2-4 Research Procedure
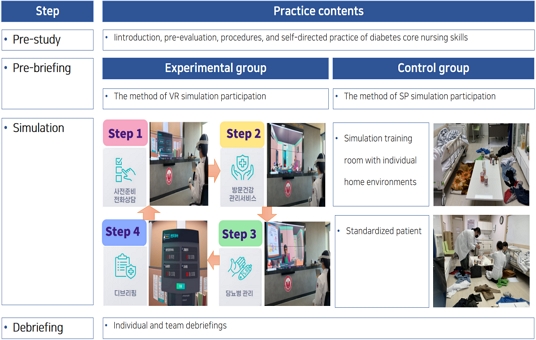
In this study, we applied the diabetes home-visiting healthcare simulation education program[5] using HMD-based VR simulation. The simulation curriculum was developed based on the NLN Jeffries simulation theory[24]. The detailed intervention contents are as follows.
The first stage was pre-study, which lasted 3 hours. This stage included program introduction, pre-evaluation, procedures for the diabetes home health management program, and self-directed practice of diabetes core nursing skills.
The second stage was a pre-briefing, which lasted 40 minutes. In this stage, the method of simulation participation, the purpose of the simulation exercise, information on the participants, division of roles, and evaluation methods were explained.
The third phase was a simulation run, which lasted a total of 20 minutes. The experimental group participated in a diabetes home-visiting healthcare simulation education program using HMD-based VR, and the control group received the same education program in a simulation training room with individual home environments where SP were placed. To ensure that the diabetes home health management practice using VR simulation applied to the experimental group can proceed smoothly, we prepared a safe space where the HMD VR device can be checked and VR can be implemented, and a nurse waiting area and rest area where emergency treatment is possible in case of adverse reactions such as dizziness or motion sickness. The educational content for diabetes home-visiting healthcare using VR simulation was developed by Ha et al[5]. To ensure that the simulation practice room with individual homes featuring SP applied to the control group can run smoothly, SP education and community simulation room environment inspections were prepared to ensure that there are no disruptions to the simulation practice.
The fourth stage was the debriefing stage, which lasted for two hours. The program consisted of individual and team debriefings on diabetes visit health management, an overall debriefing with the participation of all students and instructors, and feedback (Fig. 1).
2-5 Ethical Considerations
The subjects of this study were students who voluntarily participated in the survey through an announcement after receiving consent from the head of the department. The purpose and procedure of the research, anonymity and confidentiality, and the fact that there would be no disadvantages in withdrawing participation were fully explained to the participants, and they were asked to respond to the survey only if they agreed to participate in the research. In addition, they were clearly informed that there would be no disadvantages in terms of grades or grades if they did not participate in the research or withdrew midway, and that there would be no benefits in terms of grades or grades to the participants. A small reward was provided to the subjects who participated in the research.
2-6 Data Analysis
Data analysis was performed using the SPSS PC+ 29.0 program.
1) The general characteristics of the experimental and control groups were analyzed using frequencies, percentages, means, and standard deviations. Homogeneity of general characteristics and dependent variables between groups was tested using Fisher's exact test and independent t-tests.
2) The effect of the diabetes home-visiting healthcare simulation education program using VR according to the intervention was analyzed using two independent t-test and paired t-test.
Ⅲ. Results
3-1 Homogeneity of General Characteristics
There were no statistically significant differences between the experimental and the control groups in demographic and baseline characteristics including gender, friendship satisfaction, satisfaction with major, satisfaction with clinical practice, necessity of chronic disease home-visiting healthcare simulation classes, and family history of diabetes (Table 1).
3-2 Homogeneity Test of Dependent Variables
There were no statistically significant differences between the experimental and the control groups in the dependent variables, including learning immersion, clinical judgment ability, and clinical competency, indicating that homogeneity between the groups was secured before the implementation of the program (Table 2).
3-3 Research Hypothesis Verification
Hypothesis 1: The experimental group receiving the VR simulation-based chronic disease home-visiting healthcare simulation education program is expected to exhibit significantly different learning immersion scores compared to the control group receiving SP-based simulation. Hypothesis 1 was rejected (Table 3). The experimental group showed a statistically significant improvement in learning immersion (t=7.64, p<.001), with a post-test mean score of 76.85 (±5.11), compared to the pre-test score. The control group showed a statistically significant improvement in learning immersion in simulation (t=4.57, p<.001), with a post-test mean score of 72.97 (±7.06), compared to the pre-test score. However, the difference between the two groups after the intervention was not statistically significant (t=1.55, p=.127).
Hypothesis 2: The experimental group is expected to exhibit significantly different clinical judgment ability scores compared to the control group. Hypothesis 2 was supported (Table 3). The experimental group showed a statistically significant improvement in clinical judgment ability, with a post-test mean score of 42.24 (±2.91), compared to the pre-test score (t=6.45, p<.001). The control group also demonstrated a statistically significant increase, with a post-test mean score of 40.69 (±4.11), compared to the pre-intervention score (t=2.87, p=.008). Moreover, the difference between the two groups after the intervention was statistically significant (t=2.49, p=.015).
Hypothesis 3: The experimental group is expected to exhibit significantly different clinical competency scores compared to the control group. Hypothesis 3 was rejected (Table 3). The experimental group showed a statistically significant improvement in clinical competency, with a post-test mean score of 163.18 (±11.22), compared to the pre-test score (t=6.98, p<.001). The control group also demonstrated a statistically significant increase, with a post-test mean score of 157.31 (±14.54) (t=4.14, p<.001). However, the difference between the two groups after the intervention was not statistically significant (t=1.92, p=.060).
Ⅳ. Discussion and Conclusion
This study was conducted to compare the effects of SP simulation and VR simulation teaching methods in order to identify effective educational strategies for community health nursing practicum among nursing students.
As a result of this study, both the experimental group and the control group showed statistically significant improvements in simulation learning immersion after the intervention. However, the difference between the two groups before and after the intervention was not statistically significant. This indicates that both VR simulation and SP simulation education are effective in enhancing learning immersion.
Previous studies verifying the effectiveness of VR simulation education for hospitalization management[25], systematic reviews[26], supported the results of this study by showing that VR simulation education significantly improved learning immersion. VR is a learning tool that provides learners with experiences similar to clinical environments through three-dimensional visualizations[27]. However, some studies have reported that learners may experience decreased immersion due to cybersickness during VR simulation experiences[15]. Cybersickness results from a mismatch between visual cues and bodily movements, often causing symptoms such as dizziness, nausea, and decreased concentration[15]. In this study, participants were briefed on the potential for cybersickness prior to the simulation, allowing them to anticipate and manage any symptoms. The VR content was designed to minimize rapid screen transitions and complex interfaces, reducing sensory conflicts. Participants were also encouraged to report discomfort during the simulation, enabling the researcher to adjust pacing and interactions accordingly. These precautions and responsiveness to feedback likely contributed to enhanced learning immersion.
Studies utilizing SP simulation practice[6],[28] have reported that learning immersion in simulation significantly increased after the intervention, supporting the results of this study. SP-based simulation is an instructional method that provides realistic clinical scenarios; however, it has been shown that poorly trained SP can reduce learner immersion[6]. Therefore, in this study, detailed scenario guidelines were provided to SP prior to the simulation to enhance their understanding and proficiency, which is believed to have facilitated learner immersion.
In a previous study on nursing skill simulation[15], the conventional simulation group did not show a significant improvement in learning immersion compared to the VR simulation group, which is consistent with the findings of the present study. Furthermore, a qualitative study comparing experiences with VR simulation and SP simulation[29] highlighted that each approach possesses unique strengths and limitations. Participants noted that SP simulation provided a high degree of realism through facial expressions, nonverbal cues, and natural interactions, but also pointed out that inconsistent acting performance or exaggerated responses in certain situations could reduce learners’ immersion. Conversely, VR simulation enhanced immersion by allowing learners to intuitively perceive surrounding contexts during interactions; however, the lack of physical contact and the monotony of patients’ facial expressions and responses led some learners to perceive it as less realistic. Taken together, these findings confirm that both VR and SP simulation are effective educational strategies for enhancing learning immersion, yet each method has inherent limitations. Therefore, when designing simulation-based education, it is important to consider learning objectives and the educational environment, applying the two approaches in a complementary manner. Moreover, enhancing the realism of VR technology and strengthening the standardization of SP training may serve as effective strategies for maximizing learner immersion.
As a result of this study, clinical judgment ability significantly improved in both the experimental and control groups after the intervention, with the experimental group showing a statistically greater improvement compared to the control group. This indicates that simulation education using both VR and SP is effective in enhancing clinical judgment ability, with VR-based education demonstrating superior effectiveness. A previous study analyzing the effects of simulation education using the same measurement tool as this study reported a large effect size of 2.39[16]. Studies applying VR simulation[30] and mixed reality simulation[7] also showed significant improvements in clinical judgment ability, supporting the results of this study. Similarly, studies employing SP simulation[31],[32] reported significant enhancements in clinical judgment ability, supporting the findings of the present study.
In a study directly comparing VR simulation and SP simulation[33], although different measurement tools were used, the group that received VR simulation education demonstrated greater improvement in clinical judgment scores, supporting the findings of the present study. Most prior studies have analyzed the effects of VR simulation in experimental groups without control groups or compared high-fidelity simulation with VR simulation, limiting direct comparison with this study. However, in studies comparing high-fidelity and VR simulations[7],[30], groups using high-fidelity simulation showed greater improvements in clinical judgment ability than those using VR simulation, which contrasts with the findings of the present study.
According to a learner experience analysis study[30], while learners using VR simulation tended to concentrate on scoring based on true/false choices, limiting their engagement with the decision-making process itself. However, another study[29] reported that VR simulation provided a safe learning environment that allowed learners to make decisions actively without fear of making mistakes. Therefore, the VR simulation applied in this study was designed not to be limited to simple true/false problem-solving but to reflect the subcomponents of clinical judgment ability. Learners applied VR simulation in this study comprehensively assessed the home-visiting healthcare environment and diabetic patients, interpreted their assessments, performed appropriate nursing education, and engaged in feedback and reflection processes following the simulation. Through this comprehensive experience, learners are thought to have effectively acquired decision-making skills. Accordingly, future research should analyze the subcomponents of clinical judgment ability and apply them to each stage of simulation education.
As a result of this study, both the experimental group showed statistically significant clinical competency after the intervention. However, the difference between the two groups before and after the intervention was not statistically significant.
In this study, the experimental group that received VR simulation demonstrated a significant improvement in clinical competency after the intervention. While direct comparisons are limited due to the use of different measurement tools, these findings are consistent with previous single-group pre-post studies[17],[34],[35] reporting statistically significant improvements in clinical competency among nursing students following simulation education.
The control group, which received SP simulation, also showed improvements in clinical competency scores. Previous studies evaluating standardized simulation programs similarly reported significant improvements in clinical competency, supporting the educational value of SP simulation[36]. A previous study on a SP simulation learning module for COVID-19 patient care reported that the experimental group, which received simulation education, showed significantly greater improvement in clinical competency[37].
When comparing the two groups, no statistically significant difference was observed in overall clinical competency immediately post-intervention, although the experimental group tended to demonstrate slightly higher improvements. Most previous studies have primarily analyzed the effects of VR simulation in single-group designs without control groups, which limits direct comparisons. Nevertheless, a prior study directly comparing VR simulation with online and offline simulation programs[11] reported higher improvements in clinical performance in the VR simulation group, a finding that contrasts with the results of the present study and suggests the need for further verification. Therefore, follow-up studies are warranted that systematically compare the effects of various simulation modalities, including high-fidelity simulation, SP simulation, hybrid simulation, and VR simulation. Such studies are expected to provide critical evidence for delineating the strengths and limitations of each simulation approach, thereby contributing to the development of more effective instructional designs and implementation strategies.
The results of this study indicate that both VR simulation education and SP simulation education are effective interventions for enhancing nursing students’ competencies in diabetes home-visiting healthcare, including learning immersion in simulation, clinical judgment ability, and clinical competency. Notably, this study supports the development of VR simulation as an effective alternative to SP education, especially in limited clinical exposure environments. Furthermore, this study provides foundational data for the development and implementation of educational programs aimed at enhancing diabetes home-visiting healthcare competencies and, consequently, improving community health outcomes, thereby offering institutional and policy implications. The HMD-based VR simulation was designed with an intuitive interface that does not disrupt learners’ immersion and a detailed reproduction of actual clinical environments to enable repetitive practice. This design allowed learners to maintain high levels of engagement while simultaneously enhancing practical skills. These design principles are significant as they provide a developmental framework for improving the technical quality of VR-based education and expanding the diversity of educational content. Moreover, the findings of this study have policy implications, suggesting that integrating VR simulation education with continuing education for public health nurses could establish a foundation for strengthening community-centered chronic disease management systems.
Based on the results of this study, the following recommendations for future research are proposed. First, since this study was conducted with nursing students from a single university located in City D, future studies including a more diverse population are needed to enhance the generalizability of the findings. Second, this study evaluated the effects of each intervention immediately after its implementation. Therefore, further research is needed to examine the long-term effects of virtual reality simulation training and SP simulation training in order to assess the sustainability of their outcomes. Third, reflecting the social demand for diabetes care in the community, it is important to conduct follow-up studies to verify the effectiveness of these educational programs not only for nursing students but also for home-visiting healthcare personnel to strengthen their competencies in diabetes nursing. Such studies would provide essential institutional and policy-based evidence for strengthening the community health care system.
Acknowledgments
This research was supported by the National Research Foundation of Korea(NRF) grant funded by the Korea government(MSIT) (No. 2021R1F1A1063210).
References
- Korea Helath Statistics. Korea National Health and Nutrition Examination Survey 2023 [Internet]. Available: http://knhanes.kdca.go.kr/, .
-
S. Y. Ryu, S. W. Choi, S. J. Jeong, and H. M. Gu, “Time Series Changes in Indices of Diabetes Management from the 2008–2022 Korea Community Health Survey,” Journal of Agricultural Medicine and Community Health, Vol. 49, No. 3, pp. 179-193, September 2024.
[https://doi.org/10.5393/JAMCH.2024.49.3.179]

-
S. Y. Kim, “Management of Diabetes in the Elderly,” The Journal of Korean Diabetes, Vol. 23, No. 2, pp. 128-132, June 2022.
[https://doi.org/10.4093/jkd.2022.23.2.128]

-
M. K. Park, H. K. Park, H. J. Kim, O. J. Kim, and M. Y. Gong, “Health Management Experience of Residents through Participation in the Community-Based Hypertension and Diabetes Registry Program,” Journal of Korean Academy of Community Health Nursing, Vol. 32, No. 4, pp. 518-528, December 2021.
[https://doi.org/10.12799/jkachn.2021.32.4.518]

-
Y. S. Ha, Y. K. Park, H. S. Byun, and M. J. Choi, “Development of Virtual Reality-Based Home-Visiting Healthcare Education Content,” Journal of Digital Contents Society, Vol. 26, no. 1, pp. 1-10, January 2025.
[https://doi.org/10.9728/dcs.2025.26.1.1]

-
H. J. Choi, “The Effect of Simulation Practice Using Standardized Patients on Communication Skills, Empathy, Learning Immersion, and Learning Satisfaction,” The Journal of Learner-Centered Curriculum and Instruction, Vol. 24, No. 15, pp. 293-303, 2024.
[https://doi.org/10.22251/jlcci.2024.24.15.293]

-
E. Jung, S. Hwang, Y. Jeon, M. Lee, S. Jang, and Y. Jung, “Development and Effectiveness Evaluation of Mixed Reality-Based Nursing Simulation Training Program for Major Trauma Patient,” Korean Journal of Military Nursing Research, Vol. 41, No. 4, pp. 19-38, December 2023.
[https://doi.org/10.31148/kjmnr.2023.41.4.19]

-
H.-J. Cho and K.-S. Chong, “Effects of Community Nursing Simulation Education on Nursing Core Competencies, Clinical Judgment, and Clinical Performance of Nursing College Students,” European Journal of Investigation in Health, Psychology and Education, Vol. 15, No. 6, 92, 2025.
[https://doi.org/10.3390/ejihpe15060092]

-
A. E. Cortés-Rodríguez, P. Roman, M. M. López-Rodríguez, I. M. Fernández-Medina, C. Fernández-Sola, and J. M. Hernández-Padilla, “Role-play Versus Standardised Patient Simulation for Teaching Interprofessional Communication in Care of the Elderly for Nursing Students,” Healthcare, Vol. 10, No. 1, 46, January 2022.
[https://doi.org/10.3390/healthcare10010046]

-
W. J. Brown and R. A. W. Tortorella, “Hybrid Medical Simulation - A Systematic Literature Review,” Smart Learning Environments, Vol. 7, 16, June 2020.
[https://doi.org/10.1186/s40561-020-00127-6]

-
M. K. Ahn and C. M. Lee, “Development and Effects of Head-Mounted Display-Based Home-Visits Virtual Reality Simulation Program for Nursing Students,” Journal of Korean Academy of Nursing, Vol. 51, No. 4, pp. 465-477, August 2021.
[https://doi.org/10.4040/jkan.21051]

-
A. B. Wolf, “The Impact of Web-Based Video Lectures on Learning in Nursing Education: An Integrative Review,” Nursing Education Perspectives, Vol. 39, No. 6, pp. E16-E20, December 2018.
[https://doi.org/10.1097/01.NEP.0000000000000389]

-
J. Y. Ha, H. J. Park, and M. Kim, “Systematic Review of Immersive Simulation for Nursing Students,” Global Health and Nursing, Vol. 14, No. 1, pp. 22-36, January 2024.
[https://doi.org/10.35144/ghn.2024.14.1.22]

- E. J. Ko, The Development and Validation of a Learning Immersion in Simulation Scale, Ph.D. Dissertation, Hallym University, Chuncheon, 2020.
-
A. Jung, E. Kwon, and J. Seo, “Effects of Nursing Skills Simulation Program Using Virtual Reality (VR) on Learning Flow, Nursing Skills Confidence, Nursing Skills Performance and Usability Verification,” Journal of Korea Academia-Industrial Cooperation Society, Vol. 23, No. 11, pp. 127-135, November 2022.
[https://doi.org/10.5762/KAIS.2022.23.11.127]

-
J. M. Park and S. Jun, “The Effects of Simulation-Based Education on the Communication and Clinical Judgment of Nursing Students and Nurses: A Systematic Review and Meta-Analysis,” Journal of Korean Academic Society of Nursing Education, Vol. 29, No. 3, pp. 203-224, August 2023.
[https://doi.org/10.5977/jkasne.2023.29.3.203]

-
H. Kang and H.-Y. Kang, “The Effects of Simulation Education on Nursing Students’ Clinical Reasoning Ability, Clinical Performance, and Learning Satisfaction,” Journal of the Korea Academia-Industrial Cooperation Society, Vol. 21, No. 8, pp. 107-114, August 2020.
[https://doi.org/10.5762/KAIS.2020.21.8.107]

-
D. Han and G. J. An, “Experiences of Nursing Students with Virtual Reality-Based Anatomy Education in Korea: A Qualitative Content Analysis,” Journal of Korean Biological Nursing Science, Vol. 27, no. 1, pp. 157-167, February 2025.
[https://doi.org/10.7586/jkbns.25.002]

-
E. A. Ji, “Effects of Head-Mounted Display (HMD)-Based Virtual Reality Simulation and a Blended Education Program on Neonatal Birth Nursing,” The Journal of Learner-Centered Curriculum and Instruction, Vol. 24, No. 4, pp. 705-718, February 2024.
[https://doi.org/10.22251/jlcci.2024.24.4.705]

-
K. Lasater, “Clinical Judgment Development: Using Simulation to Create an Assessment Rubric,” Journal of Nursing Education, Vol. 46, No. 11, pp. 496-503, 2007.
[https://doi.org/10.3928/01484834-20071101-04]

-
K. Shim and H. Shin, “The Reliability and Validity of the Lasater Clinical Judgement Rubric in Korean Nursing Students,” Child Health Nursing Research, Vol. 21, No. 2, pp. 160-167, April 2015.
[https://doi.org/10.4094/chnr.2015.21.2.160]

- W. H. Lee, C. J. Kim, J. S. Yoo, H. K. Hur, K. S. Kim, and S. M. Lim, “Development of a Clinical Competency Measurement Tool for Students,” Yonsei Journal of Nursing, Vol. 13, pp. 17-29, 1990.
-
B. Y. Kim, M. J. Chae, and Y. O. Choi, “Reliability and Validity of the Clinical Competency Scale for Nursing Students,” Research in Community and Public Health Nursing, Vol. 29, No. 2, pp. 220-230, June 2018.
[https://doi.org/10.12799/jkachn.2018.29.2.220]

-
P. R. Jeffries, B. Rodgers, and K. Adamson, “NLN Jeffries Simulation Theory: Brief Narrative Description,” Nursing Education Perspectives, Vol. 36, No. 5, pp. 292-293, 2015.
[https://doi.org/10.1097/00024776-201509000-00004]

-
Y.-J. Kim, “Development and Application of Scenario-based Admission Management VR Contents for Nursing Students,” Journal of the Korea Society of Computer and Information, Vol. 26, No. 1, pp. 209-216, January 2021.
[https://doi.org/10.9708/jksci.2021.26.01.209]

-
S. Shorey and E. D. Ng, “The Use of Virtual Reality Simulation among Nursing Students and Registered Nurses: A Systematic Review,” Nurse Education Today, Vol. 98, 104662, March 2021.
[https://doi.org/10.1016/j.nedt.2020.104662]

-
K. Koo, T. Park, H. Jeong, S. Khang, C. S. Koh, M. Park, ... and J. Lee, “Simulation Method for the Physical Deformation of a Three Dimensional Soft Body in Augmented Reality-Based External Ventricular Drainage,” Healthcare Informatics Research, Vol. 29, No. 3, pp. 218-227, 2023.
[https://doi.org/10.4258/hir.2023.29.3.218]

-
Y. G. Bak and T. K. Kim, “The Effect of Simulation-Based Education Using a Standardized Patients for Schizophrenia Nursing Care on Communication Self-Efficacy, Learning Self-Efficacy and Flow Experience in Nursing Students,” Asia-Pacific Journal of Multimedia Services Convergent with Art, Humanities, and Sociology, Vol. 8, No. 6, pp. 437-447, 2018.
[https://doi.org/10.35873/ajmahs.2018.8.6.040]

-
N. Harder, F. Ali, S. Turner, K. Workum, and L. Gillman, “Comparing Artificial Intelligence-Enhanced Virtual Reality and Simulated Patient Simulations in Undergraduate Nursing Education,” Clinical Simulation in Nursing, Vol. 105, 101780, August 2025.
[https://doi.org/10.1016/j.ecns.2025.101780]

-
E. H. Lee and S. Y. Ryu, “Analysis of the Virtual Simulation Practice and High Fidelity Simulation Practice Training Experience of Nursing Students: A Mixed-Methods Study,” The Journal of Korean Academic Society of Nursing Education, Vol. 27, No. 3, pp. 227-239, August 2021.
[https://doi.org/10.5977/jkasne.2021.27.3.227]

-
S. O. Shin, “The Effects of Smoker Nursing Simulation Module Practice on Communication Self-Efficacy, Clinical Judgement and Learning Satisfaction for Nursing Students,” Journal of the Korea Entertainment Industry Association, Vol. 12, No. 8, pp. 357-363, December 2018.
[https://doi.org/10.21184/jkeia.2018.12.12.8.357]

-
M.-R. Eom, H.-S. Kim, E.-K. Kim, and K. Seong, “Effects of Teaching Method Using Standardized Patients on Nursing Competence in Subcutaneous Injection, Self-Directed Learning Readiness, and Problem Solving Ability,” Journal of Korean Academy of Nursing, Vol. 40, No. 2, pp. 151-160, April 2010.
[https://doi.org/10.4040/jkan.2010.40.2.151]

-
G. S. Karaduman and T. Basak, “Is Virtual Patient Simulation Superior to Human Patient Simulation: A Randomized Controlled Study,” CIN: Computers, Informatics, Nursing, Vol. 41, No. 6, pp. 467-476, June 2023.
[https://doi.org/10.1097/CIN.0000000000000957]

-
K.-J. Kim, Y.-S. Ha, and Y.-K. Park, “The Effects of Virtual Simulation Program-Based Convergence Action Learning on Problem-Solving, Critical Thinking, Communication Skills, and Clinical Competency of Nursing Students,” Journal of the Korea Convergence Society, Vol. 13, No. 5, pp. 489-499, May 2022.
[https://doi.org/10.15207/JKCS.2022.13.05.489]

-
O. S. Lee, “The Effect of Simulation-Based Practical Education on Nursing Students’ Critical Thinking Disposition, Communication Ability, and Clinical Performance,” Journal of the Korea Academia-Industrial Cooperation Society, Vol. 18, No. 4, pp. 93-100, April 2017.
[https://doi.org/10.5762/KAIS.2017.18.4.93]

-
B. J. Koo, “Effect of Online Nursing Practical Education Program on Learning Self-Efficacy, Clinical Performance, and Learning Satisfaction of College Students,” Journal of Wellness, Vol. 17, No. 3, pp. 203-210, August 2022.
[https://doi.org/10.21097/ksw.2022.8.17.3.203]

-
Y.-E. Kim and H.-Y. Kang, “Effects of a Nursing Simulation Learning Module on Clinical Reasoning Competence, Clinical Competence, Performance Confidence, and Anxiety in COVID-19 Patient-Care for Nursing Students,” Journal of Korean Academy of Nursing, Vol. 53, No. 1, pp. 87-100, 2023.
[https://doi.org/10.4040/jkan.22130]

저자소개

2014년 8월:경북대학교 간호학과 (간호학박사)
2018년 3월~현 재: 경일대학교 간호대학 교수
※관심분야:가상현실, 생성형AI, 시뮬레이션, 만성질환

2015년 2월:경북대학교 간호학과 (간호학박사)
2016년 3월~현 재: 경일대학교 간호대학 교수
※관심분야:중환자간호, 간호교육, 시뮬레이션, 환자안전, 의료질관리(QI)

2005년 2월:경북대학교 간호학과 (간호학박사)
2013년 9월~현 재: 영남이공대학교 간호학과 교수
※관심분야:지역사회간호, 학교보건, 노인간호, 종양환자간호

2018년:경북대학교 일반대학원 (간호학 박사)
2022년 9월~현 재: 경북대학교 간호대학 교수
※관심분야:시뮬레이션, 간호교육, 위기관리, 재난간호

2020년 8월:경북대학교 간호학과 (간호학박사)
2021년 3월~현 재: 경일대학교 간호대학 교수
※관심분야:가상현실, 시뮬레이션, 아동청소년간호, 정신간호